What is Eczema, or Dermatitis, Involving the Skin of the Eyelids (also known as Periocular Eczema and Periocular Dermatitis)?
Eczema, or dermatitis, involving the skin of the eyelids is known as periocular eczema, periocular dermatitis, or periocular atopic dermatitis.
Periocular eczema, or periocular dermatitis, is:
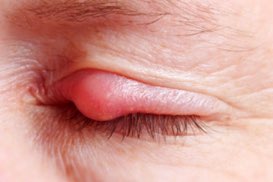
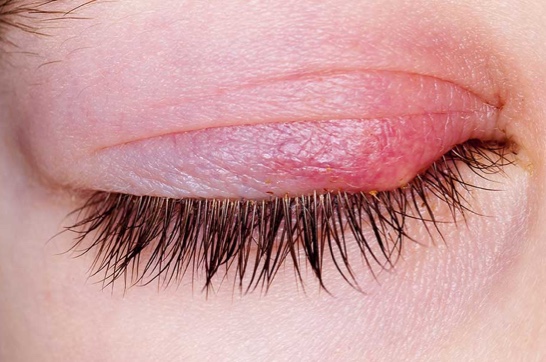
- Characterized by inflammation of the skin of the eyelids.
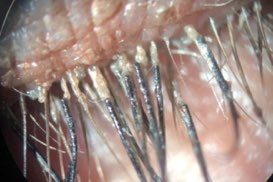
- Patients present with scaly, erythematous and/or hyperpigmented eyelids, often with wrinkled, crepey skin changes.
- Patients complain of redness, itching and burning of their eyes and/or eyelids.
- Eczema or dermatitis of the eyelids is a chronic condition characterized by periods of remission and exacerbation/flares.
- Left untreated, eczema and dermatitis of the eyelids can result in long-term architectural changes and induration, or thickening, of the eyelids and unwanted skin changes.
- Eczema and dermatitis of the eyelids is usually associated with, or exacerbated by, allergies (food allergies, environmental allergies, and/or chemical allergies). Eczema or dermatitis of the eyelids is often associated with the following medical conditions: asthma, post-nasal drip (PND), sinusitis, and atopy/allergies.
Allergic Contact Dermatitis is a common cause of eczema and/or dermatitis involving the skin of the eyelids (also known as periocular eczema, or periocular dermatitis).
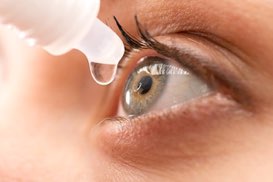
Allergic Contact Dermatitis can be caused by a variety of allergens including preservatives often found in eye drops, ingredients commonly found in cosmetics, shampoos, conditioners, lotions, laundry detergents, etc.
Airborne Contact Dermatitis is a subset of allergic contact dermatitis, with the distinction that the allergen is a volatile, or aerosolized, substance.
This can include fragrances, perfumes, scents from candles, air fresheners, nail polish, paint fumes, and glues, as well as innumerable natural and synthetic substances that may be encountered in daily life.
Because much of the rest of the body’s skin is thicker, and/or covered by clothing, the periocular skin (skin of the eyelids) is often the only skin affected.
Both Allergic and Airborne Contact Dermatitis may also be triggered by plant or animal proteins, such as pollens, dust mites, and/or animal dander.
Airborne allergens are a common cause of eczema and/or dermatitis involving the skin of the eyelids (also known as periocular eczema, or periocular dermatitis).
How do you Diagnose Eczema and/or Dermatitis Involving the Skin of the Eyelids (also known as Periocular Eczema, or Periocular Dermatitis)?
The diagnosis of eczema and/or dermatitis involving the skin of the eyelids is made by reviewing the patient’s medical history and examining the patient’s eyes, and the skin of his/her eyelids, with a biomicroscope.
Next, allergy testing, including environmental, food, and chemical allergy patch testing, is performed to identify allergens that may be contributing to, or exacerbating, the patient’s periocular eczema/periocular dermatitis, and other associated medical conditions such as asthma, post-nasal drip (PND) and sinusitis.
How do you Treat Eczema and/or Dermatitis Involving the Skin of the Eyelids (also known as Periocular Eczema, or Periocular Dermatitis)?
- Avoidance of allergens identified via allergy testing (environmental, food and chemical).
- Moisturizing the skin around the eyes with fragrance-free moisturizers, or organic, cold-pressed castor oil.
- Applying cold gel packs to closed eyes (cold is a natural anti-inflammatory) for symptomatic relief.
- Antihistamine eye drops and nasal spray, to be used on an as-needed basis for relief of allergy symptoms.
- Immunotherapy:
- Via Sublingual Immunotherapy, or SLIT, which involves simply placing a few drops under your tongue once a day in the comfort and privacy of your own home, or via weekly allergy shots. Both methods are completely customizable and can be used to desensitize an individual to his/her allergens to reduce symptoms and inflammation on future exposure to said allergen.
- Topical corticosteroids in the form of both eye drops and/or ophthalmic ointment; oral steroids can be used in moderate-severe cases.
- Restasis drops (a calcineurin inhibitor) prescribed to be taken from 2-8x/day.
- Applying topical medications containing calcineurin inhibitors:
- Tacrolimus drops 0.03%
- Tacrolimus ophthalmic ointment 0.03% (or 0.1%)
- Dupixent for Moderate-Severe Eczema:
- Food and Drug Administration (FDA) approved, injectable medication.
- Studies have shown it to be safe when used as directed.
- Dupixent is a prescription medication used to reduce the inflammation associated with moderate-to-severe atopic dermatitis. It is not a steroid, and therefore avoids the risks, and the broad immunosuppression, associated with the use of systemic steroids. However, it can be used along with steroids, if needed.
- Dupixent is a biologic; specifically, a monoclonal antibody which targets two key mediators of inflammation, thereby reducing inflammation, thus breaking the itch-scratch cycle, and in that way decreasing the incidence of infections in/of the skin.
- Dupixent is self-administered via a subcutaneous injection into either the thigh, or the abdomen, using a 200 mg, or a 300 mg, pre-filled pen.
- One dose is administered, most commonly, every 2 weeks following the initial loading dose.
- Dosage is based upon age and weight.